Prostate cancer represents a significant health challenge for men globally. Understanding its early symptoms and the diverse array of available treatments is crucial for timely intervention and improved outcomes. This guide explores the multifaceted landscape of Prostate Cancer Symptoms & Treatments, offering a comprehensive, fact-based overview.
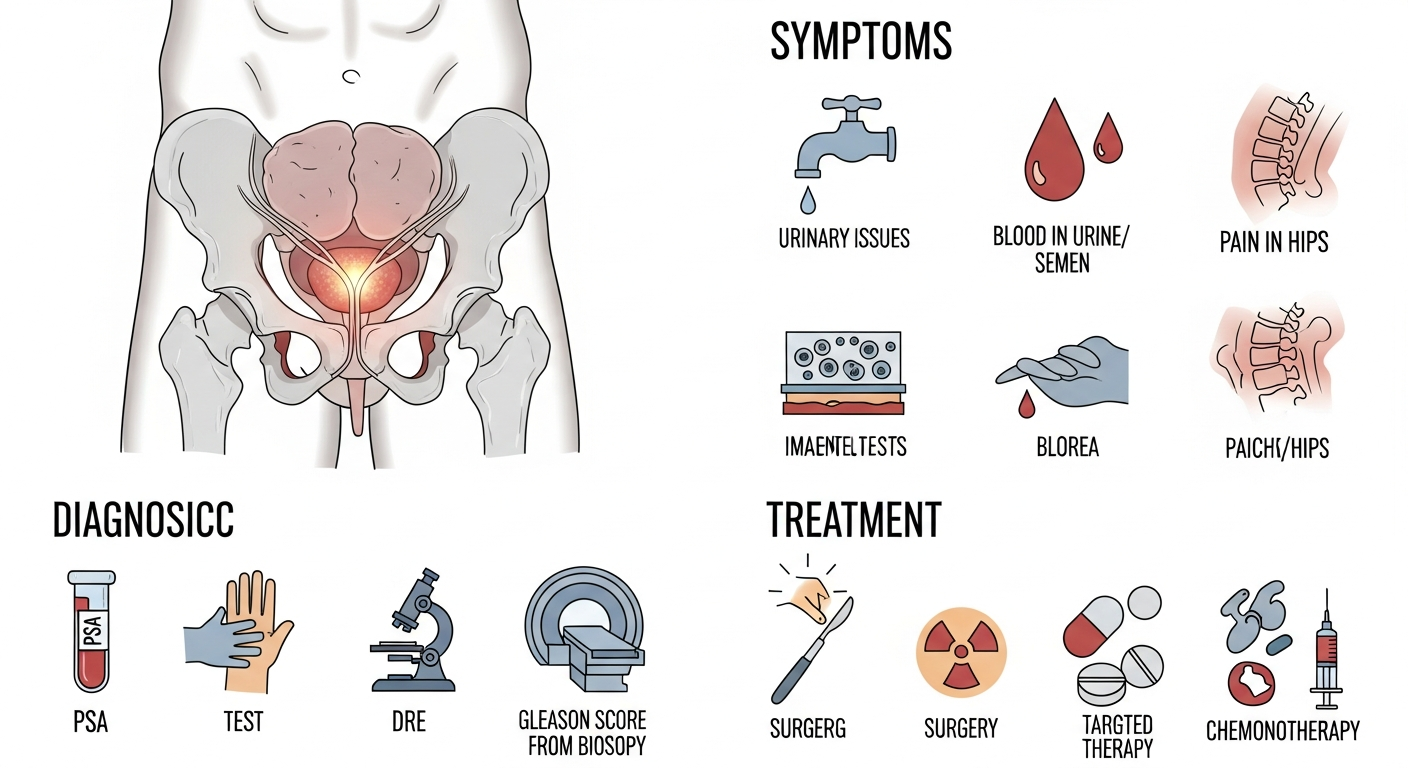
The Prostate Gland and Cancer Development
The prostate is a small, walnut-sized gland located just below the bladder in men, surrounding the urethra. Its primary function is to produce seminal fluid, which nourishes and transports sperm. Prostate cancer occurs when cells in the prostate gland grow abnormally and uncontrollably. While many prostate cancers grow slowly and may not cause significant harm, others can be aggressive and spread rapidly.
Several factors are recognized as increasing the risk of prostate cancer. Age is the most prominent risk factor, with the majority of diagnoses occurring in men over 65. Ethnicity also plays a role; men of African descent have a higher incidence and mortality rate from prostate cancer. A family history of the disease, particularly in a father or brother before age 65, significantly increases an individual’s risk. Genetic mutations, such as those in the BRCA1 or BRCA2 genes, are also associated with an elevated risk, though these account for a smaller percentage of cases.
Recognizing Prostate Cancer Symptoms
One of the challenging aspects of prostate cancer is that in its early stages, it often presents with no discernible symptoms. This asymptomatic phase underscores the importance of screening discussions between patients and healthcare providers. When symptoms do emerge, they can vary widely and may overlap with other benign conditions, such as benign prostatic hyperplasia (BPH) or infections.
Common Symptoms, Especially in Advanced Stages:
- Urinary Difficulties: As the prostate gland enlarges due to cancer, it can press on the urethra, leading to a range of urinary issues. These may include frequent urination, particularly at night (nocturia), a weak or interrupted urine flow, difficulty starting or stopping urination, and a feeling of incomplete bladder emptying. While these are common Prostate Cancer Symptoms & Treatments considerations, they are also frequently associated with BPH, a non-cancerous enlargement of the prostate.
- Blood in Urine or Semen: Although less common, the presence of blood in urine (hematuria) or semen (hematospermia) can be a symptom of prostate cancer. However, these symptoms can also result from infections, kidney stones, or other conditions.
- Pain or Discomfort: In more advanced stages, when prostate cancer has spread beyond the prostate, it can cause pain. This pain often manifests in the lower back, hips, or pelvis. Bone pain is particularly concerning as the bones are common sites for prostate cancer metastasis.
- Erectile Dysfunction: Difficulty achieving or maintaining an erection can be a symptom of prostate cancer, especially if the cancer affects nerves responsible for erectile function. However, erectile dysfunction has numerous causes, including age, other medical conditions, and lifestyle factors.
- Unexplained Weight Loss and Fatigue: As with many other cancers, advanced prostate cancer can lead to general symptoms such as unexplained weight loss, loss of appetite, and persistent fatigue.
It is crucial to understand that the presence of one or more of these symptoms does not definitively mean an individual has prostate cancer. Many conditions can cause similar symptoms. Therefore, any new or concerning symptoms warrant a consultation with a healthcare professional for proper evaluation and diagnosis. This careful assessment is part of the comprehensive approach to understanding Prostate Cancer Symptoms & Treatments.
Diagnosis and Staging of Prostate Cancer
Accurate diagnosis and staging are fundamental steps in determining the most appropriate Prostate Cancer Symptoms & Treatments plan. This process typically involves a combination of screening tests, physical examinations, and more definitive diagnostic procedures.
Screening for Prostate Cancer:
- Prostate-Specific Antigen (PSA) Test: The PSA test measures the level of PSA, a protein produced by prostate cells, in the blood. Elevated PSA levels can indicate prostate cancer, but they can also be raised by other conditions like BPH, prostate infection (prostatitis), or recent prostate irritation. The decision to undergo PSA screening is complex and should involve a detailed discussion with a doctor about potential benefits and risks, including the possibility of false positives or overdiagnosis and overtreatment of clinically insignificant cancers.
- Digital Rectal Exam (DRE): During a DRE, a doctor manually examines the prostate through the rectum to feel for any abnormalities in shape, size, or texture, such as lumps or hard areas, that might suggest cancer.
The timing and frequency of screening recommendations vary based on individual risk factors and guidelines from different medical organizations.
Diagnostic Procedures:
- Prostate Biopsy: If screening tests suggest the possibility of cancer, a biopsy is typically recommended. This procedure involves taking small samples of prostate tissue, usually guided by transrectal ultrasound (TRUS) or increasingly, by MRI-guided or transperineal approaches. The tissue samples are then examined by a pathologist under a microscope to confirm the presence of cancer cells.
- Gleason Score: The pathologist assigns a Gleason score to the cancer based on the architectural patterns of the cancer cells. This score, ranging from 6 to 10, indicates how aggressive the cancer appears. A lower score (e.g., 6) suggests a less aggressive cancer, while a higher score (e.g., 8-10) indicates more aggressive disease.
- Imaging Tests: Once cancer is confirmed, imaging tests may be performed to determine if the cancer has spread outside the prostate (staging). These can include magnetic resonance imaging (MRI) of the prostate, CT scans of the abdomen and pelvis, bone scans to check for spread to bones, and sometimes PET scans.
Staging Prostate Cancer:
Prostate cancer is staged using the TNM system (Tumor, Nodes, Metastasis), which describes the extent of the primary tumor (T), whether the cancer has spread to nearby lymph nodes (N), and whether it has spread to distant parts of the body (M). This staging, combined with PSA levels and Gleason score, helps classify the cancer into risk groups (e.g., very low, low, intermediate, high, very high risk) which are critical for guiding Prostate Cancer Symptoms & Treatments decisions.
Prostate Cancer Treatments: A Comprehensive Overview
The selection of Prostate Cancer Symptoms & Treatments is a highly individualized process, tailored to the specific characteristics of the cancer, the patient’s overall health, age, life expectancy, and personal preferences regarding potential side effects. A multidisciplinary team of specialists often collaborates to formulate the most appropriate plan.
Watchful Waiting and Active Surveillance:
- Active Surveillance: For men with very low-risk or low-risk localized prostate cancer, active surveillance is often a recommended approach. This involves close monitoring of the cancer through regular PSA tests, DREs, and repeat biopsies. The goal is to avoid or delay aggressive treatments and their associated side effects for cancers that are unlikely to cause harm, while still being prepared to intervene if the cancer shows signs of progression.
- Watchful Waiting: This approach is typically considered for older men or those with significant co-existing health conditions who have a limited life expectancy. It involves monitoring symptoms and providing palliative treatment if the cancer progresses, but without curative intent.
Localized Treatments (for cancer confined to the prostate):
-
- Surgery (Radical Prostatectomy): This procedure involves the surgical removal of the entire prostate gland, along with seminal vesicles and sometimes nearby lymph nodes. It can be performed through traditional open surgery, laparoscopically, or with robotic assistance. Potential side effects include urinary incontinence and erectile dysfunction, the severity of which can vary.
- Radiation Therapy: This treatment uses high-energy rays to kill cancer cells.
- External Beam Radiation Therapy (EBRT): Radiation is delivered from a machine outside the body. Advanced techniques like Intensity-Modulated Radiation Therapy (IMRT) and Stereotactic Body Radiation Therapy (SBRT) allow for more precise targeting of the prostate while minimizing damage to surrounding healthy tissues.
- Brachytherapy (Internal Radiation Therapy): Radioactive seeds are permanently or temporarily placed directly into the prostate gland, delivering a high dose of radiation to the cancer while sparing surrounding organs.
Side effects of radiation therapy can include urinary, bowel, and sexual problems, which may develop during or after treatment.
- Focal Therapy: Emerging treatments such as High-Intensity Focused Ultrasound (HIFU) or cryotherapy aim to destroy only the cancerous parts of the prostate while preserving healthy tissue. These are typically considered for highly selected cases of localized disease.
Systemic Treatments (for advanced or metastatic cancer):
When prostate cancer has spread beyond the prostate, systemic treatments are often necessary to target cancer cells throughout the body. These are key components of addressing advanced Prostate Cancer Symptoms & Treatments.
-
- Hormone Therapy (Androgen Deprivation Therapy – ADT): Prostate cancer cells often rely on male hormones (androgens, primarily testosterone) to grow. Hormone therapy aims to reduce the levels of androgens in the body or block their action.
- LHRH Agonists/Antagonists: These medications reduce testosterone production by the testicles.
- Antiandrogens: These drugs block the ability of cancer cells to use androgens.
- Hormone Therapy (Androgen Deprivation Therapy – ADT): Prostate cancer cells often rely on male hormones (androgens, primarily testosterone) to grow. Hormone therapy aims to reduce the levels of androgens in the body or block their action.
Side effects of hormone therapy can include hot flashes, fatigue, loss of libido, erectile dysfunction, weight gain, bone thinning, and muscle loss.
- Chemotherapy: Chemotherapy drugs work by killing rapidly dividing cells, including cancer cells. It is typically used for prostate cancer that has spread and no longer responds to hormone therapy (castration-resistant prostate cancer). Common chemotherapy regimens involve drugs administered intravenously. Side effects vary but can include fatigue, nausea, hair loss, and increased risk of infection.
- Targeted Therapy: These drugs target specific molecules or pathways involved in cancer growth and survival. For example, PARP inhibitors may be used for men with advanced prostate cancer who have certain genetic mutations, such as BRCA1 or BRCA2.
- Immunotherapy: Immunotherapy drugs work by stimulating the body’s own immune system to recognize and destroy cancer cells. While less broadly applicable than for some other cancers, specific immunotherapy agents are approved for certain types of advanced prostate cancer, particularly in the castration-resistant setting.
- Radiopharmaceuticals: These are radioactive drugs that are injected into the bloodstream and travel to cancer cells, delivering radiation directly to them. An example includes radium-223 for bone metastases.
Emerging Treatments and Clinical Trials:
The field of prostate cancer research is dynamic, with ongoing development of new therapies and approaches. Participation in clinical trials can offer access to cutting-edge Prostate Cancer Symptoms & Treatments that are not yet widely available. Patients are encouraged to discuss this option with their healthcare team.
Palliative Care:
For men with advanced prostate cancer, palliative care plays an essential role in managing symptoms, improving quality of life, and providing support for both the patient and their family. Palliative care can be integrated at any stage of the disease, alongside curative treatments.
Personalized Treatment Approach
It is paramount to reiterate that there is no one-size-fits-all approach to Prostate Cancer Symptoms & Treatments. The optimal treatment strategy is carefully determined through a comprehensive evaluation that considers numerous factors:
- Cancer Characteristics: This includes the stage of the cancer (how far it has spread), the grade (Gleason score), and the PSA level.
- Patient Factors: The patient’s age, overall health status (presence of other medical conditions), life expectancy, and personal values and preferences regarding potential side effects and quality of life are crucial.
- Shared Decision-Making: Patients are encouraged to engage actively in discussions with their healthcare team, weighing the potential benefits and risks of each treatment option. This shared decision-making process ensures that the chosen plan aligns with the individual’s goals and priorities.
The complexity of Prostate Cancer Symptoms & Treatments underscores the importance of a coordinated approach involving urologists, radiation oncologists, medical oncologists, pathologists, and other specialists.
Conclusion
The journey through Prostate Cancer Symptoms & Treatments is often complex and highly individualized. Continuous advancements in medical science offer a broader spectrum of diagnostic tools and therapeutic options, improving outlooks for many. Understanding these facets empowers individuals and their families to engage more effectively with healthcare providers in managing this condition.
