Lung cancer remains a significant global health challenge. Understanding the array of available lung cancer treatment options is crucial for those affected and their support networks. This guide provides an objective overview of current medical strategies employed in managing this complex disease, offering insight into the diverse pathways of care.
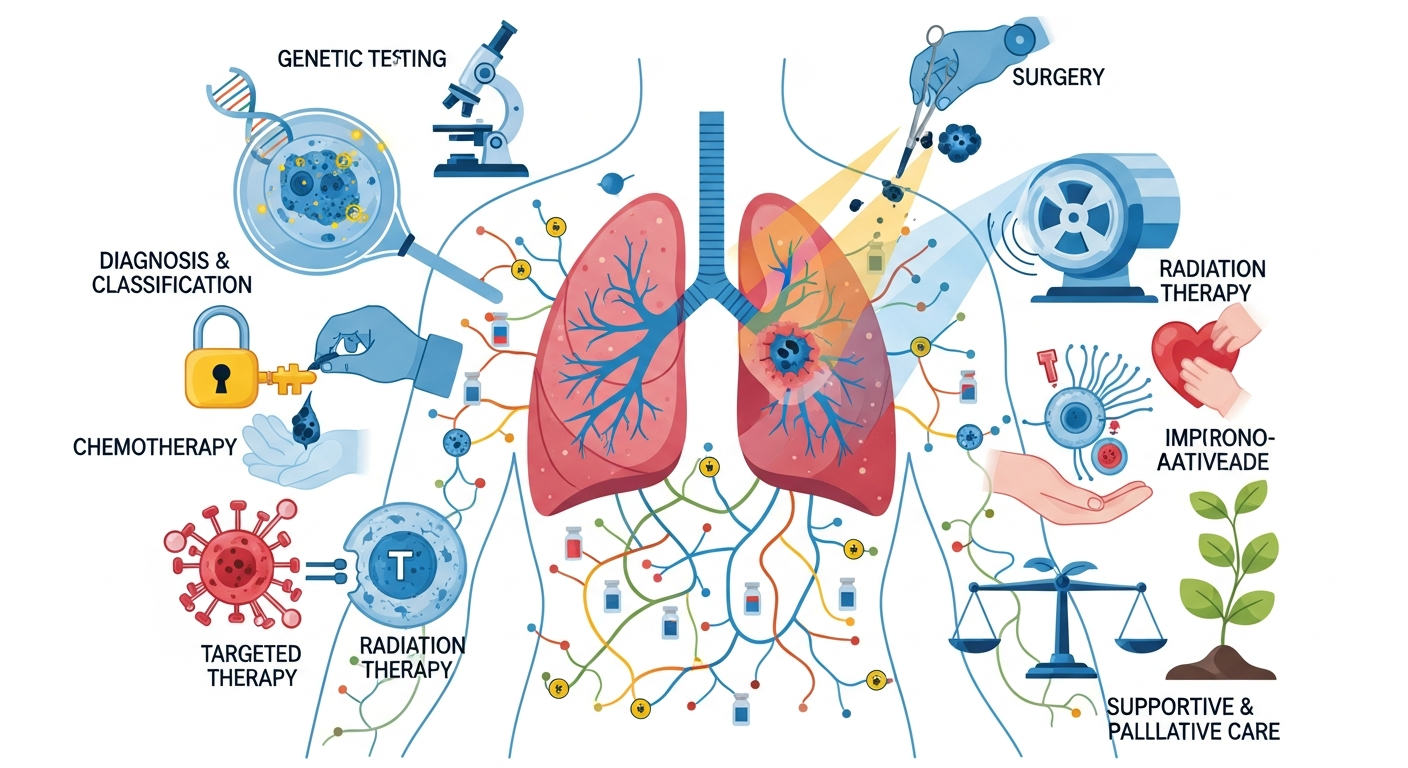
The Foundations of Lung Cancer Treatment: Diagnosis and Classification
Before any lung cancer treatment plan can be established, an accurate diagnosis and detailed staging are paramount. Lung cancer is broadly categorized into two main types: Non-Small Cell Lung Cancer (NSCLC), which accounts for approximately 85% of cases, and Small Cell Lung Cancer (SCLC), comprising the remaining 15%. These classifications are critical because they dictate fundamentally different approaches to lung cancer treatment due to their distinct biological behaviors and responses to therapies.
Diagnosis typically involves imaging tests, biopsies, and often advanced molecular testing to identify specific genetic mutations or biomarkers. The stage of the cancer – whether it is localized, locally advanced, or has metastasized – is another pivotal factor that profoundly influences the choice and intensity of lung cancer treatment. This detailed understanding allows medical teams to tailor the most appropriate and effective strategies for each individual.
Pillars of Modern Lung Cancer Treatment Modalities
The landscape of lung cancer treatment has evolved significantly, moving beyond conventional methods to incorporate advanced, targeted approaches. Current treatment strategies often involve a multidisciplinary approach, combining several modalities to achieve the best possible outcomes. These pillars include surgical intervention, radiation therapy, chemotherapy, targeted therapy, and immunotherapy, each playing a distinct role in addressing the disease depending on its type and stage.
The selection of a particular lung cancer treatment, or a combination thereof, is a complex decision, informed by a patient’s overall health, the specific characteristics of their cancer, and a comprehensive evaluation by an expert medical team. Advances in research continually refine these options, offering new hope and improved prospects for patients diagnosed with lung cancer.
Surgical Intervention for Lung Cancer
Surgery stands as a primary curative option for early-stage Non-Small Cell Lung Cancer (NSCLC) when the tumor is localized and can be entirely removed. The extent of the surgical procedure depends on the size and location of the tumor, as well as the patient’s lung function and overall health. Common surgical procedures include:
- Lobectomy: Removal of an entire lobe of the lung, the most common type of lung cancer surgery.
- Pneumonectomy: Removal of an entire lung, typically reserved for larger or centrally located tumors.
- Wedge Resection or Segmentectomy: Removal of a smaller section of the lung, used for very small tumors or when a patient’s lung function is compromised.
Surgical intervention may also be followed by adjuvant therapy, such as chemotherapy or radiation, to eliminate any remaining cancer cells and reduce the risk of recurrence. The feasibility and type of surgery are carefully considered as part of the overall lung cancer treatment plan by a thoracic surgeon in consultation with the oncology team.
Radiation Therapy in Lung Cancer Management
Radiation therapy utilizes high-energy rays to damage and destroy cancer cells. It is a versatile component of lung cancer treatment, employed in various scenarios for both NSCLC and SCLC:
- Curative intent: For early-stage NSCLC in patients who are not candidates for surgery, or as part of definitive chemoradiation for locally advanced NSCLC.
- Adjuvant therapy: After surgery to eliminate residual cancer cells.
- Neoadjuvant therapy: Before surgery to shrink tumors and make them easier to remove.
- Palliative care: To alleviate symptoms such as pain, bleeding, or obstruction caused by the tumor.
Technological advancements have led to more precise forms of radiation, such as Stereotactic Body Radiation Therapy (SBRT), which delivers high doses of radiation to a small, localized tumor with minimal impact on surrounding healthy tissue. Proton therapy is another advanced option gaining traction. The planning and delivery of radiation are highly individualized to maximize its effectiveness as a lung cancer treatment while minimizing side effects.
Chemotherapy: A Systemic Approach
Chemotherapy involves the use of powerful drugs to kill cancer cells throughout the body. It is a systemic lung cancer treatment, meaning the drugs travel through the bloodstream to target cancer cells wherever they may be. Its role varies significantly depending on the type and stage of lung cancer:
- Small Cell Lung Cancer (SCLC): Chemotherapy is often the primary treatment for SCLC, frequently combined with radiation therapy due to its aggressive and fast-spreading nature.
- Non-Small Cell Lung Cancer (NSCLC):
- Adjuvant: Given after surgery to destroy any remaining cancer cells.
- Neoadjuvant: Administered before surgery to shrink tumors.
- Palliative: Used in advanced stages to control disease progression and manage symptoms, improving quality of life.
Chemotherapy is often given in cycles, with periods of treatment followed by periods of rest. While effective, it can cause side effects by affecting healthy, fast-growing cells in the body. The specific drugs and regimen are chosen based on the cancer type, stage, and the patient’s overall health and tolerance to ensure the most effective lung cancer treatment.
Targeted Therapy: Precision in Lung Cancer Treatment
Targeted therapy represents a significant advancement in personalized lung cancer treatment. Unlike traditional chemotherapy, these drugs specifically target molecular pathways or proteins that are crucial for cancer cell growth and survival, while largely sparing healthy cells. This approach requires specific genetic testing of the tumor tissue to identify particular biomarkers or mutations.
For Non-Small Cell Lung Cancer (NSCLC), common targets include:
- EGFR mutations: Epidermal Growth Factor Receptor inhibitors.
- ALK rearrangements: Anaplastic Lymphoma Kinase inhibitors.
- ROS1 rearrangements: ROS1 inhibitors.
- BRAF mutations: BRAF inhibitors.
- RET rearrangements, MET alterations, HER2 mutations, KRAS mutations: Emerging targets with specific inhibitors.
By precisely interfering with these pathways, targeted therapies can offer more effective lung cancer treatment with often fewer systemic side effects compared to conventional chemotherapy. These therapies are typically administered orally and have significantly improved outcomes for patients with specific genetic alterations, marking a paradigm shift in how lung cancer is managed.
Immunotherapy: Harnessing the Body’s Defenses
Immunotherapy is a revolutionary form of lung cancer treatment that empowers the patient’s own immune system to recognize and destroy cancer cells. Cancer cells often develop ways to evade immune detection, and immunotherapies, particularly checkpoint inhibitors, work by blocking these evasion mechanisms.
Key types of immunotherapy used in lung cancer include:
- PD-1/PD-L1 inhibitors: These drugs block the PD-1 (programmed cell death protein 1) or PD-L1 (programmed death-ligand 1) pathway, which cancer cells use to switch off immune responses. By unblocking this pathway, the immune system can effectively attack the cancer.
- CTLA-4 inhibitors: Another class of checkpoint inhibitors that block the CTLA-4 protein, also involved in regulating T-cell activity.
Immunotherapy is increasingly used in both early and advanced stages of NSCLC, sometimes as a first-line lung cancer treatment, either alone or in combination with chemotherapy. It has also shown promise in SCLC. While it can lead to durable responses in some patients, it also carries its own unique set of immune-related side effects, which require careful monitoring. Its introduction has significantly broadened the arsenal of effective lung cancer treatment options.
Small Cell Lung Cancer (SCLC) Treatment Specifics
Small Cell Lung Cancer (SCLC) is distinct from NSCLC due to its aggressive nature and rapid growth. Consequently, the lung cancer treatment approach for SCLC differs significantly:
- Limited Stage SCLC: For cancer confined to one side of the chest that can be encompassed within a single radiation field, the primary lung cancer treatment often involves concurrent chemotherapy and radiation therapy. This intensive approach aims for cure. Prophylactic cranial irradiation (PCI) may also be recommended to prevent brain metastases, a common occurrence in SCLC.
- Extensive Stage SCLC: For cancer that has spread more widely, systemic chemotherapy is the cornerstone of lung cancer treatment. While historically the prognosis has been challenging, the integration of immunotherapy alongside chemotherapy has shown improved outcomes in recent years, offering new hope.
Due to its rapid growth and tendency to metastasize early, surgery is rarely a primary treatment for SCLC unless it’s a very early-stage presentation or a unique clinical scenario. Research continues to explore more effective and less toxic lung cancer treatment strategies for SCLC.
Factors Influencing Lung Cancer Treatment Decisions
The selection of the most appropriate lung cancer treatment is a highly individualized process, guided by a multitude of factors. A multidisciplinary team of specialists, including oncologists, pulmonologists, radiation oncologists, and surgeons, collaborates to formulate a comprehensive plan. Key considerations include:
- Type and Stage of Cancer: As discussed, NSCLC and SCLC have different treatment paradigms, and the stage (localized, regional, or metastatic) profoundly impacts options.
- Molecular Characteristics: For NSCLC, the presence of specific genetic mutations (e.g., EGFR, ALK) is critical for targeted therapy eligibility.
- Patient’s Overall Health and Performance Status: Coexisting medical conditions, age, and general physical fitness influence tolerance to aggressive treatments.
- Lung Function: Important for assessing suitability for surgery or certain radiation techniques.
- Treatment Goals: Whether the aim is curative, to prolong life, or to manage symptoms (palliative care).
- Patient Preferences and Values: Informed patient input is vital in shared decision-making.
This holistic assessment ensures that the chosen lung cancer treatment strategy is not only medically sound but also aligned with the patient’s individual circumstances and priorities.
Emerging Horizons in Lung Cancer Treatment
The field of lung cancer treatment is in constant evolution, driven by relentless scientific inquiry and technological advancements. Research continues to unveil deeper insights into the molecular underpinnings of the disease, paving the way for novel therapeutic strategies. Some key areas of ongoing development include:
- Novel Targeted Therapies: Development of new drugs that target a broader array of genetic alterations and resistance mechanisms.
- Advanced Immunotherapy Approaches: Exploring combination immunotherapies, bispecific antibodies, and cellular therapies to enhance immune responses against cancer.
- Liquid Biopsies: Non-invasive blood tests for early detection, monitoring treatment response, and detecting resistance mutations.
- Artificial Intelligence and Machine Learning: Being integrated into diagnosis, treatment planning, and drug discovery to personalize lung cancer treatment further.
- Minimally Invasive Techniques: Advances in robotic surgery and advanced interventional pulmonology procedures.
Participation in clinical trials offers access to these cutting-edge therapies and contributes significantly to the progression of lung cancer treatment. These ongoing efforts underscore a future where lung cancer management is increasingly precise, effective, and tailored to the individual.
Supportive and Palliative Care: An Integral Component
While active lung cancer treatment focuses on combating the disease, supportive and palliative care are equally critical components of a comprehensive treatment plan. These services aim to prevent and alleviate suffering and improve the quality of life for patients and their families, from diagnosis through treatment and survivorship. This is not just for end-of-life care but throughout the entire cancer journey.
Key aspects of supportive and palliative care include:
- Symptom Management: Addressing pain, fatigue, nausea, shortness of breath, and other physical symptoms.
- Nutritional Support: Guidance to maintain strength and manage treatment side effects.
- Psychological and Emotional Support: Counseling, support groups, and resources to help cope with the emotional impact of a cancer diagnosis.
- Spiritual Care: Addressing spiritual or existential concerns.
- Physical Therapy and Rehabilitation: To maintain mobility and function.
Integrating palliative care early into the lung cancer treatment process has been shown to improve both quality of life and, in some cases, survival. It ensures that patients receive holistic care that addresses all aspects of their well-being.
Conclusion
The field of lung cancer treatment is dynamic, characterized by continuous research and evolving therapeutic strategies. From traditional approaches like surgery, radiation, and chemotherapy to innovative targeted therapies and immunotherapies, the goal remains to improve patient outcomes and quality of life. Understanding these diverse options, alongside the critical role of supportive care, is key to navigating the complexities of this disease and highlights the personalized nature of modern oncology.
